Ovarian cancer is the 5th most common cause of cancer death in women, and while it is not the most common cancer, it is deadly. At the time of diagnosis, over 55% of patients have metastasis, and this relates to only a 32% 5-year survival rate (data from SEER Cancer Stat Facts). However, detecting the disease when it is still localized translates to a 91.7% 5-year survival rate.
Over 324,000 new cases were reported in 2022. As the Global Cancer Observatory graphic shows, the incidence is not uniform worldwide. What is quite common, though, worldwide is a late diagnosis of patients with ovarian cancer. Due to a lack of specific symptoms and non-invasive to minimally invasive early detection methods, most cases are diagnosed in the late stages of the disease. This greatly limits the ability to successfully treat the disease.
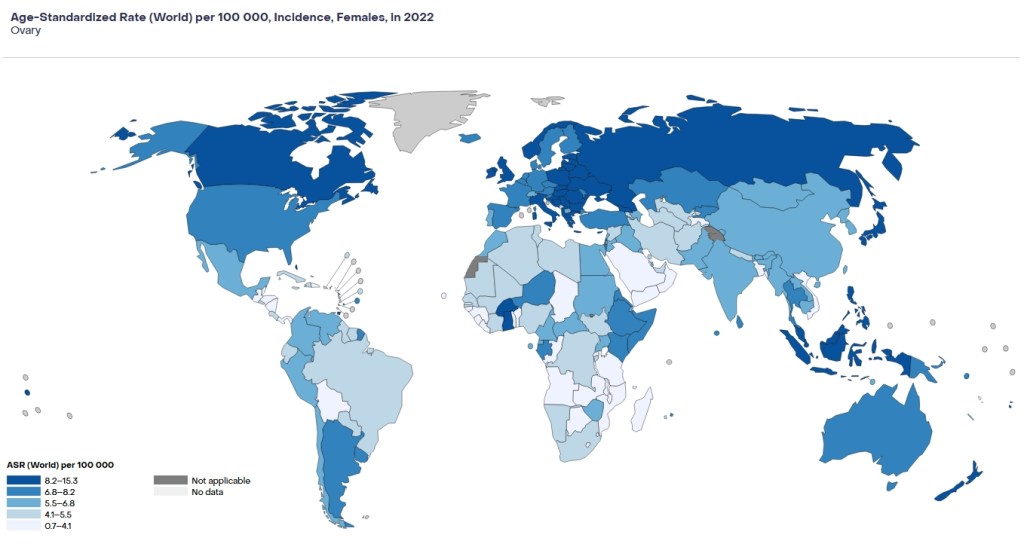
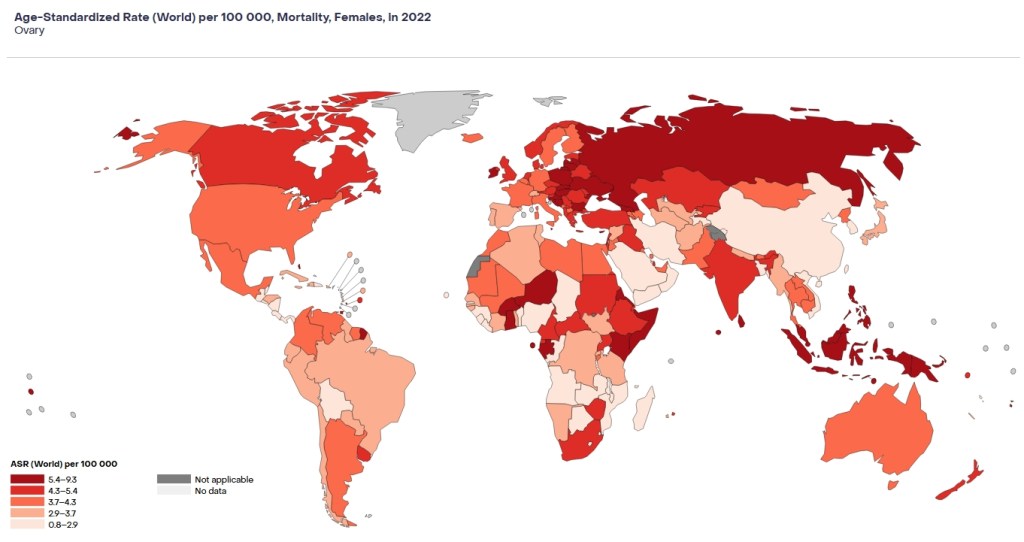
So, what are the symptoms of ovarian cancer?
- Pelvic or abdominal pain, can be combined with discomfort or bloating
- Getting full quickly when eating
- Fatigue
- Weight loss
- Abnormal bleeding or vaginal discharge
- Changes in your bowel habits – diarrhea or constipation
- Size increase of your abdomen
- More frequent urination
These symptoms can be a warning sign of an ovarian cancer. Your doctor should investigate what is the cause of the anomalies. If you have a familiy history of ovarian cancer, Lynch syndrome or inherited a pathogenic variant in BRCA1 or BRCA2 gene, your risk can be higher. In general risk of ovarian cancer increases with age (risk is higher for those over 60 years of age), suffering from endometriosis, not being pregnant, being overweight or obese. This list is not exhaustive but it includes commonly accepted risks.
There are ongoing efforts to create a better early diagnostic test, that will allow to detect ovarian cancer at an early stage without a need for a surgical intervention. Currently, a combination of blood tests (e.g. CA-125 blood test) and imaging tests (e.g. transvaginal ultrasound) is done to diagnose the disease but definitive diagnosis is performed during a surgery.
Treatment options will depend on an individual cancer and stage at diagnosis. If you have been diagnosed with an ovarian cancer, it is important that you receive genetic testing. Such testing can guide your treatment (e.g. PARP inhibitors if BRCA mutations are found) but also identify a hereditary cancer risk in your family. This is important since the variants in BRCA1 and BRCA2 can cause other cancers (e.g. breast, pancreatic, prostate, or melanoma). NCCN guidelines recommend germline and cancer (or somatic) genetic testing , however, it appears that only just over 50% of patients receive it.
Genetic testing faces multiple barriers:
- Lack of recommendation by the physician
- Lack of insurance coverage for genetic testing of patient
- Incorrect testing performed
- Out-of-pocket costs of testing
- Access to a genetic counseling services without the need for separate appointment
As a patient you need to ask about the genetic testing, if it is covered and what was and was not tested. Ask to speak to a genetic counselor. The way your medical care is managed will depend on the insurance you have, state you live in, or country you live in. That said most clinicians are familiar with NCCN guidelines. As the diagnosis can be very stressful, take a family member or a friend to an appointment and make sure that they ask all the questions on your behalf if you find it too overwhelming.
References:
- SEER Cancer Stat Facts: ovarian cancer. https://seer.cancer.gov/statfacts/html/ovary.html (accessed 14 May 2025)
- https://my.clevelandclinic.org/health/diseases/4447-ovarian-cancer
- https://www.mayoclinic.org/diseases-conditions/ovarian-cancer/symptoms-causes/syc-20375941
- https://www.cancer.org/cancer/types/ovarian-cancer/about.html
- https://www.cancer.gov/types/ovarian
- https://www.patientpower.info/news/ovarian-cancer/too-many-ovarian-cancer-patients-missing-out-on-life-changing-genetic-testing


Leave a comment